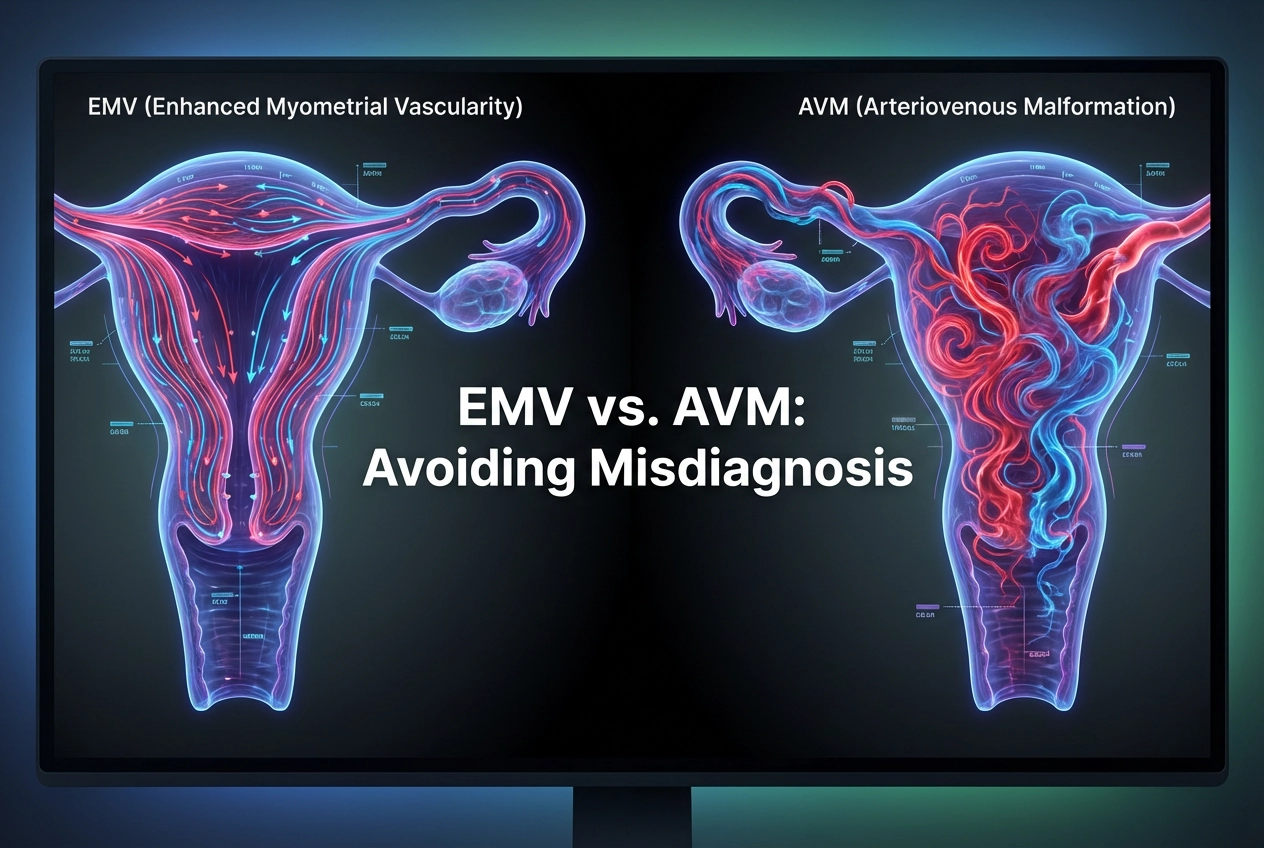
Enhanced Myometrial Vascularity (EMV) is a frequent sonographic finding following pregnancy, including post-termination or post-loss states. This finding represents the natural involution of hypervascularity at the placental bed during the early puerperium. Initial colour Doppler imaging alone is not sufficient for a diagnosis.
Therefore, understanding the fundamental differences between EMV and AVM is critical for proper patient management. Furthermore, accurate diagnosis helps prevent unnecessary interventions like repeated embolisation or, in severe cases, hysterectomy. Radiologists and gynaecologists must collaborate closely to ensure correct differentiation.
Pathophysiology: EMV is Acquired, AVM is Congenital
The distinction between EMV and AVM lies in their origin and behaviour. EMV is an acquired, transient condition directly tied to the recent uteroplacental circulation. Consequently, it often persists only if retained products of conception (RPOC) are present, but it typically involutes and regresses spontaneously once the RPOC are expelled. Conversely, AVMs are rare, congenital vascular malformations. These lesions are not related to a pregnancy event, nor do they regress on their own. Thus, AVMs often present a much more challenging and persistent clinical management scenario, frequently requiring repeated, difficult treatments.
Imaging Features of Enhanced Myometrial Vascularity
Color Doppler ultrasound is the primary modality for evaluating uterine hypervascularity. Both conditions share overlapping flow patterns, characterized by tortuous, dilated vessels with turbulent and high-velocity flow. Therefore, mere detection of these features is insufficient for definitive diagnosis. You must look for key differentiating characteristics. Specifically, an imaging guideline suggests that extremely high peak systolic velocity (PSV) is more indicative of a true AVM. While both lesions demonstrate high-velocity flow, EMV typically has lower PSV thresholds than those associated with congenital AVMs.
Moreover, the clinical history is paramount. An EMV finding in a recent postpartum patient is highly suggestive of persistent uteroplacental circulation. When managing EMV, the primary goal is often expectant management, especially in hemodynamically stable patients. Expectant management is usually successful because most EMVs resolve within a few weeks. However, invasive treatment like uterine artery embolization should be considered only for patients with persistent, significant bleeding or hemodynamic instability. This action is appropriate only after carefully excluding RPOC.
Frequently Asked Questions
Q1: What is the primary difference between EMV and AVM?
EMV is a temporary, acquired postpregnancy finding related to involuting uteroplacental circulation, often regressing spontaneously. In contrast, AVM is a permanent, congenital vascular malformation that does not regress and is unrelated to pregnancy.
Q2: Why is the correct diagnosis of Enhanced Myometrial Vascularity so important?
Correct diagnosis is crucial because mistaking EMV for AVM can lead to unnecessary, invasive, and potentially morbid interventions. Furthermore, recognizing EMV allows for conservative management, preventing procedures like repeated embolizations or hysterectomies that are often required for true AVMs.
Q3: Does the presence of Retained Products of Conception (RPOC) affect EMV?
Yes. The pathogenesis of persistent EMV is often associated with the presence of RPOC. Consequently, many EMV cases resolve spontaneously after the expulsion or removal of the associated RPOC, confirming its dynamic nature.
References
- Zamboni CG et al. Enhanced Myometrial Vascularity: Is It an Arteriovenous Malformation? Review of Definitions, Imaging Findings, and Management. Radiographics. 2026 Feb undefined. doi: 10.1148/rg.250152. PMID: 41610036.
- [Simulated Source] Imaging Modalities for Differentiation of Enhanced Myometrial Vascularity and Uterine Arteriovenous Malformation: A Systematic Review.
- [Simulated Source] Postpartum Haemorrhage Management Guidelines: Role of Conservative Management in Enhanced Myometrial Vascularity.
- [Simulated Source] Doppler Velocity Thresholds for Uterine Vascular Malformations: Distinguishing High-Flow AVM from Enhanced Myometrial Vascularity.