Emergency Medicine (EM) remains one of the most dynamic and high-impact medical specialities, requiring practitioners to make rapid, accurate decisions often under severe time constraints. The unpredictable nature of emergencies is such that every case can be radically different, from cardiac arrests and major trauma to complex poisonings and mass casualty incidents. As the landscape of acute care continues to evolve, staying ahead demands more than just theoretical knowledge; it requires mastery of specific, practice-oriented skills that ensure patient safety and optimal outcomes.
For practising MBBS and MD doctors in India, investing in the right emergency medicine skills for 2025 and beyond is not just prudent — it is an ethical imperative that directly shapes survival rates and care quality. This article highlights key competencies every modern emergency physician should develop and shows how structured training can embed these capabilities seamlessly into daily practice
The Ever-Rising Bar: Why Core Competence Matters
Emergency departments are unpredictable by nature. A physician may need to shift within moments from managing a patient in septic shock to stabilising a child with status epilepticus, all while triaging new arrivals and coordinating with multi-disciplinary teams. Such demands mean that foundational competencies must be robust, reflexive, and continually updated in line with evidence-based practice.
While certain attributes — like composure and communication — are timeless, the procedural and diagnostic toolkit of the modern emergency doctor is expanding. Here are the priority emergency medicine skills 2025 demands from well-prepared physicians.
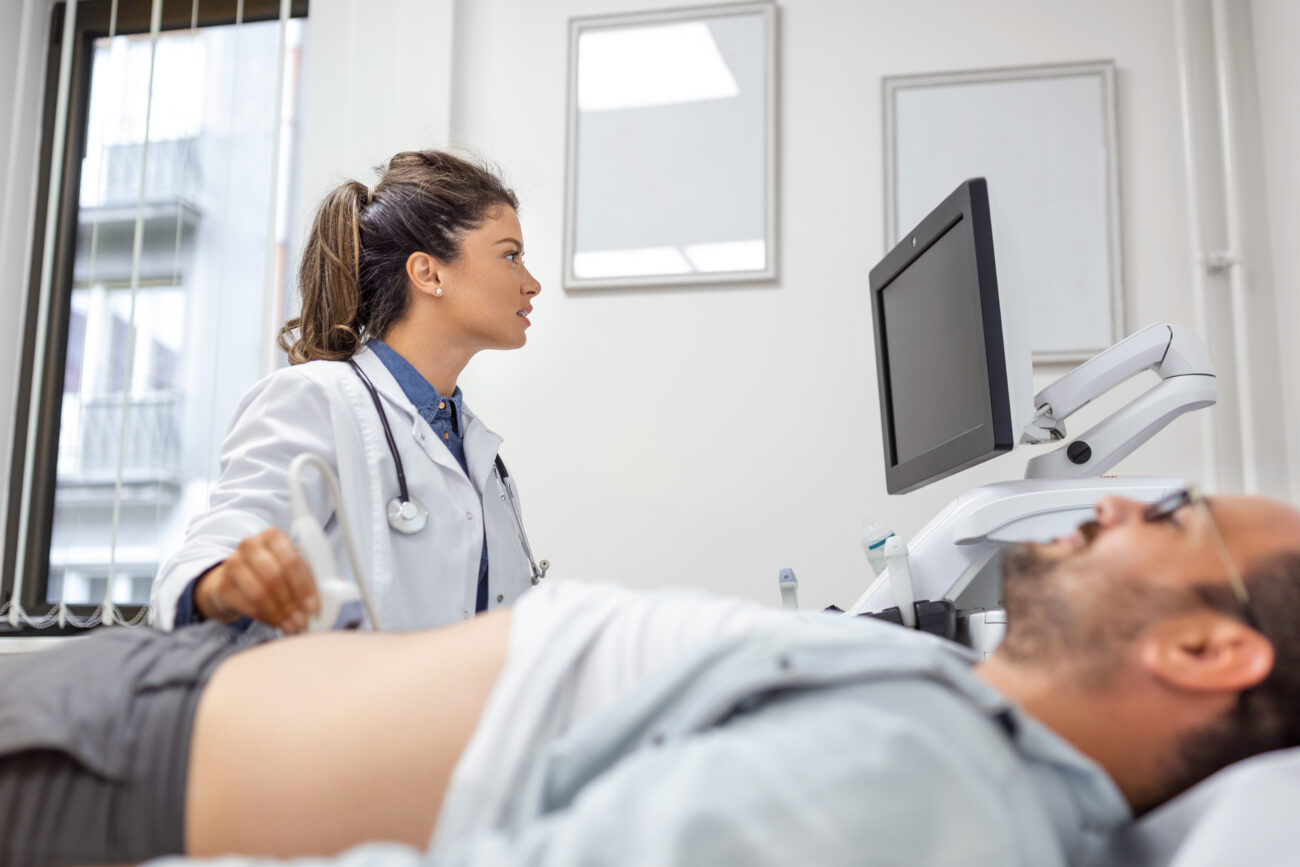
1. Point-of-Care Ultrasound (POCUS): Enhancing Bedside Decisions
Ultrasound in the emergency department is no longer a luxury; it is rapidly becoming standard practice. POCUS enables immediate, real-time visualisation of cardiac activity, abdominal bleeding, pleural fluid, and vascular access sites — all critical in time-sensitive scenarios.
For example, in a hypotensive trauma patient, a focused assessment with sonography for trauma (FAST) can quickly detect internal haemorrhage, guiding urgent surgical referral. Similarly, bedside echocardiography helps confirm tamponade or severe left ventricular dysfunction, directly influencing management.
Mastering this modality empowers physicians to supplement physical examination with precise, visual data, reducing diagnostic uncertainty and unnecessary delays. As portable ultrasound devices become more affordable, proficiency in POCUS will rank among the essential skills for emergency doctors worldwide.
2. ACLS and PALS: Universal Life Support Mastery
Advanced Cardiac Life Support (ACLS) and Paediatric Advanced Life Support (PALS) certifications are non-negotiable for any emergency physician committed to safe practice. ACLS equips doctors to manage adult cardiac arrests, lethal arrhythmias, and peri-arrest conditions confidently. Meanwhile, PALS extends this preparedness to critical paediatric scenarios such as respiratory failure and circulatory shock.
In resource-variable environments, immediate resuscitation often determines survival long before definitive specialist input arrives. Well-drilled life support protocols ensure interventions like rapid defibrillation, airway securing, and drug administration are carried out without hesitation.
Regular re-certification and scenario-based drills reinforce algorithm adherence and refine team dynamics — a proven way to mitigate human errors during high-stress resuscitations.
3. Comprehensive Trauma Management
Globally, trauma remains a leading cause of morbidity and mortality, particularly among younger populations. Managing trauma effectively goes far beyond initial wound care; it requires systematic evaluation, prioritisation, and swift decision-making that follows established frameworks such as ATLS (Advanced Trauma Life Support).
A doctor must be adept at performing primary and secondary surveys, recognising life-threatening injuries quickly, and coordinating timely surgical or critical care intervention. This includes managing airway compromise, massive haemorrhage, chest injuries, and neurotrauma.
Given the high trauma burden in India, a solid grounding in these emergency medical procedures for doctors significantly improves outcomes, especially in rural or semi-urban centres where trauma surgeons may not be immediately accessible.
For doctors keen to deepen their expertise in child-specific trauma and emergencies, pursuing a Diploma Course in Paediatric Emergency Medicine builds specialised protocols and decision-making confidence for paediatric cases.
4. Telemedicine and Remote Triage: The Digital Edge
Telemedicine has transformed routine outpatient care, and it is increasingly indispensable in acute scenarios as well. From virtual triage of accident victims in remote locations to providing guidance during disaster responses, tele-emergency care extends the reach of skilled clinicians.
Doctors proficient in telemedicine tools can coordinate ambulance crews, guide stabilisation protocols remotely, and determine the urgency of transfers, thus optimising resource use and reducing preventable deterioration.
As health systems scale up digital infrastructure, comfort with virtual consultation platforms, secure patient data sharing, and remote monitoring will become key future skills for emergency physicians who aim to deliver equitable, timely care in diverse settings.
5. Crisis Management and Leadership Under Pressure
Beyond procedures and protocols, a defining trait of an outstanding emergency physician is the ability to lead calmly in crises. Whether during mass casualty incidents, outbreaks, or internal hospital emergencies, clear-headed leadership ensures efficient resource allocation, effective team coordination, and morale retention under stress.
Modern crisis management training for physicians involves simulated disaster drills, command role rehearsals, and interdepartmental coordination exercises. Such preparation instils the confidence to prioritise actions, communicate transparently with families and staff, and de-escalate chaos into a controlled, patient-centred response.
Bridging the Gap: How OC Academy’s Training Equips Doctors for the Future
Developing these skills independently can be daunting, especially alongside busy hospital shifts and evolving clinical responsibilities. This is where structured, globally-aligned training steps in as an enabler, not a substitute for MD or DNB degrees, but a complementary catalyst for professional competence.
OC Academy’s courses for emergency medicine are designed precisely with these modern demands in mind. Each programme combines:
- In-depth Theoretical Modules: Covering POCUS techniques, trauma algorithms, telemedicine integration, and life support protocols aligned with international guidelines.
- Hands-On Clinical Observerships: Providing practical exposure in high-volume emergency departments under senior consultants.
- Authentic Scenario-Based Learning: From mock resuscitation codes to remote triage simulations, ensuring doctors translate textbook knowledge into confident bedside action.
- Expert Mentorship: Continuous guidance from experienced emergency physicians who share real-world insights and feedback, accelerating learning curves and preventing avoidable errors.
Whether preparing for MRCEM, upskilling before a fellowship abroad, or strengthening local practice, OC Academy’s pathways are flexible enough to integrate seamlessly with existing clinical commitments.
Conclusion: Investing in Skills That Save Lives
Emergency Medicine is an evolving frontier, but its core mission remains timeless — delivering timely, decisive care when lives hang in the balance. As 2025 approaches, the competencies outlined here are no longer optional extras; they are the backbone of safe, modern practice.
For MBBS graduates and early-career MD doctors, proactively developing these emergency medicine skills is a mark of commitment to patient safety, professional growth, and global readiness.
OC Academy stands as a trusted academic partner, equipping doctors with the critical thinking, procedural fluency, and leadership resilience needed to excel in emergency departments anywhere in the world.
Choosing to invest in structured, up-to-date courses for emergency medicine today is not merely a career step — it is an investment in a future defined by clinical excellence, ethical practice, and lives saved when it matters most.
FAQs
1. Is there an advanced upskilling pathway for experienced emergency doctors?
Yes. For practising MBBS and MD doctors who wish to deepen their expertise beyond core skills, enrolling in a Masters in Emergency Medicine can be a strategic upskilling choice. It builds advanced diagnostic reasoning, leadership capabilities, and exposure to global protocols, ensuring doctors stay at the forefront of modern emergency care. This programme complements existing degrees and supports career growth into senior clinical or academic roles.
2. Why is mastering POCUS becoming so important for emergency physicians?
Point-of-Care Ultrasound (POCUS) is now integral to rapid bedside decision-making. It allows immediate visual confirmation of internal injuries, cardiac activity, or fluid collections without waiting for radiology reports. For emergency doctors, proficiency in POCUS shortens diagnosis times and guides life-saving interventions when seconds matter.
3. How do ACLS and PALS certifications contribute to patient safety?
ACLS and PALS provide structured, evidence-based protocols for managing adult and paediatric emergencies. Well-trained doctors can perform high-stakes procedures — from defibrillation to advanced airway management — confidently and correctly, reducing preventable errors during cardiac arrests and respiratory crises.
4. What role does telemedicine play in modern emergency medicine practice?
Telemedicine extends emergency expertise to remote or underserved locations. It enables doctors to triage patients virtually, advise paramedics on stabilisation, and coordinate safe transfers. Especially during disasters or rural emergencies, telemedicine supports timely interventions and optimises limited resources.
5. Can structured crisis management training really improve outcomes in mass emergencies?
Yes. Crisis management drills and leadership training prepare physicians to remain calm, prioritise tasks, and coordinate teams effectively during mass casualty incidents. This preparedness reduces chaos, improves triage efficiency, and ensures that critical resources are directed where they are most needed.